3D printers: A revolutionary frontier for medicine
by Ivar Mendez — The Conversation
Mission control on earth receives an urgent communication from Mars that an astronaut has fractured his shinbone. Using a handheld scanning device, the crew takes images of his damaged tibia and transmits them to earth.
Orthopedic surgeons then use a 3D printer to create an exact replica of the astronaut’s leg from medical imaging files obtained before the voyage. Surgeons on earth use a robot to stabilize the bone with a metal plate on the 3D replica. The data is transmitted back to Mars, where surgical instruments, a personalized plate and screws are 3D printed. Finally, a surgical robot operates on the injured astronaut.
As a neurosurgeon and a researcher in remote presence robotics, I offer you this vision of the future. I am also a member of the Expert Group on the Potential Healthcare and Biomedical Roles for Deep Space Human Spaceflight of the Canadian Space Agency. Though 3D printing in space is still in early development, a revolution in 3D printing is already occurring closer to home. And it has transformative implications for the future of health care.
What is 3D printing?
Additive manufacturing, or 3D printing, uses a digital model to build an object of any size or shape — by adding successive layers of material in a single continuous run. This layering capability allows the manufacturing of complex shapes, such as the intricate structure of bones or vascular channels, that would be impossible to create by other methods.
Advances in computer design and the ability to translate medical imaging — such as X-rays, computerized tomography (CT), magnetic resonance imaging (MRI) or ultrasound — to digital models that can be read by 3D printers are expanding its applications in health care. 3D printing is opening a horizon of amazing possibilities, such as bioprinting living tissues with “biological ink.”
An advantage of 3D printing technology is that it allows for personalization of health care — customized prostheses and tailor-made drugs and organs, for example. This technology may also decrease costs by disrupting supply chains and lowering the production costs of medical devices, surgical instruments and other health-care products.
Hearing aids and dentures
At present, 3D printing is being widely used in the manufacture of hearing aids and in dentistry.
In 2013, there were 10 million 3D-printed hearing aids in circulation worldwide. This huge impact in the hearing aid industry has been called the “quiet revolution” as it has gone almost unnoticed. Before 3D printing, it took one week to manufacture a hearing aid; now it takes only a few hours.
The development of sophisticated and accurate 3D oral scanners and new 3D printing dental materials has also catapulted 3D printing as a disruptive technology in dentistry.
In 2016, the Food and Drug Administration Agency (FDA) approved 3D printing denture material and this set the stage for dentists to introduce 3D-printing manufacturing laboratories into their offices. The idea of producing crowns, orthodontic appliances or removable dentures with a push of a button in your dentist’s office is not far from reality.
Prostheses for land-mine victims
Perhaps the biggest impact of 3D printing globally could be in helping to narrow inequality in health-care delivery by producing inexpensive health-care products for low income regions. Prostheses for landmine victims is a good example.
Landmines in conflict zones in Africa and Asia have devastating consequences for the populations living in those areas. Inexpensive 3D-printed prostheses, customized to the person and printed in one day, have greatly benefited landmine amputees. Networks of volunteers such as e-NABLE and NotImpossible working with open source collaborations have had a positive impact on the design and provision of affordable 3D-printed prostheses.
In 2017 alone, these projects have created 300 prosthetic hands that have directly benefited war victims and the disabled poor.
Face transplants and spine surgery
Surgical applications of 3D printing are evolving rapidly from the production of models for surgical planning to biological active implants for craniofacial reconstruction.
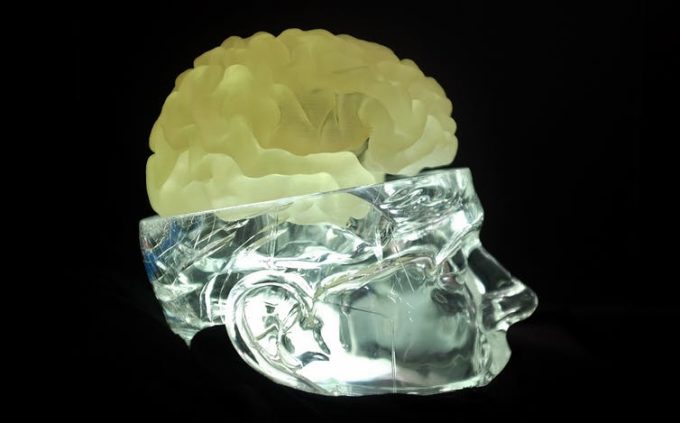
At the University of Saskatchewan, we have 3D-printed a human brain replica from MRI data. And we use it to plan complex neurosurgical procedures for treating patients with movement disorders. The surgery involves implanting electrodes that target pea-sized structures in the depths of the brain.
Surgeons have used similar 3D printed models to plan complex surgeries ranging from a full-face transplant to spine surgery. Implantable surgical devices such as the recently FDA-approved and 3D-printed titanium bone implant coated with bioactive agents that promote bone growth are also starting to reach the clinic.
Printing living organs
An exciting area with huge potential for the future is the manufacturing of 3D-printed drugs. The first 3D-printed drug approved by the FDA is the anti-seizure medication Sprintam. The 3D printing process enables the creation of a highly porous structure that can load a large dosage of the active compound into a rapidly dissolvable pill.
This possibility of highly personalized drugs, which optimize beneficial effects while reducing side effects, made in real-time using digital recipes could radically change the pharmaceutical industry.
One of the most promising 3D printing technological advances is the bioprinting of living tissue. Great strides have been made in manufacturing tissue constructs that could eventually be used for organ transplants.
The clinical manufacturing of biologically active complex structures such as functional skeletal muscle or liver tissue is promising. The recent commercialization of functional human liver or kidney constructs — the so-called “lab on a chip organ” — will have a huge impact on medical research, drug discovery and toxicology. It could possibly reduce the need to use experimental animal models.
Although we may be far away from surgery in Mars using 3D printing technology, the advances on earth are already changing health care.
Ivar Mendez is the Fred H. Wigmore Professor and Unified Head of the Department of Surgery, University of Saskatchewan
This article was originally published on The Conversation. Read the original article.
~ ~ ~
These announcements are interactive. Click on them for more information.









