A World War I soldier in France, suffering from a type of traumatic brain injury then commonly referred to as “shell shock.” US National Museum of Health and Medicine photo.
Low-level blasts from heavy weapons can cause traumatic brain injury:
two engineers explain the physics of invisible cell death
by Alice Lux Fawzi, University of Wisconsin-Madison and Christian Franck, University of Wisconsin-Madison
When the force of a blast shoots a round out of a large-caliber rifle, howitzer or M1 Abrams tank gun, the teams of people operating these weapons are exposed to low-level blasts that can cause traumatic brain injuries.
Low-level blasts do not cause visible trauma, such as bleeding from ruptured eardrums, and they don’t cause injury through violent head motion, such as a concussion. Yet, these blasts can cause physical changes in the brain that lead to a host of neuropsychiatric symptoms.
The link between the force of a blast and the resulting changes in the brain is not completely understood. So our team of engineers and scientists in the PANTHER program, funded by the Department of Defense, is using physics to elucidate how blasts cause traumatic brain injury.
What is a blast?
When a weapon like a rifle is fired, the round is initially in its barrel. Pulling the trigger engages a primer that produces a flame, igniting the propellant. This chemical reaction releases stored energy and creates high-pressure, rapidly expanding gas. This is the blast.
The rate and magnitude of gas expansion are often so extreme that they create a shock wave, where high-pressure air molecules travel outward faster than the speed of sound. This invisible pulse of high pressure carries a tremendous amount of energy. It’s the same force that can propel a 24-pound warhead out of the muzzle of a howitzer to hit a target 19 miles (30.6 kilometers) away.
 This cross-section shows: 1. bullet; 2. case; 3. gunpowder; 4. rim; and 5. primer. Glrx/Quadrell via Wikimedia Commons, CC BY-SA
This cross-section shows: 1. bullet; 2. case; 3. gunpowder; 4. rim; and 5. primer. Glrx/Quadrell via Wikimedia Commons, CC BY-SA
Linking blast to brain injury
As blast pressure enters the brain, it is initially compressive, meaning it squeezes the tissue equally from all sides. Because brain tissue is largely composed of water molecules, which are difficult to compress, this type of pressure tends to cause little known harm to cells.
An initially compressive wave, or positive pressure wave, that squeezes brain tissue changes when it bounces off the inside of the skull. It is reflected as a tensile wave, or negative pressure wave, which tends to pull brain tissue apart. With low enough pressures, micron-sized bubbles can form in a process called cavitation. These bubbles can grow 10 to 50 times their initial size over the course of less than a tenth of a millisecond, rapidly stretching the adjacent brain tissue.
Experiments from our lab have shown that the deformation caused by cavitation bubbles happens so rapidly – like the speed of a bullet – that cells tend to get torn apart. The extreme speed of stretching and squeezing causes nearby brain cells to die immediately. Afterward, we see only fragments where healthy cells used to be.
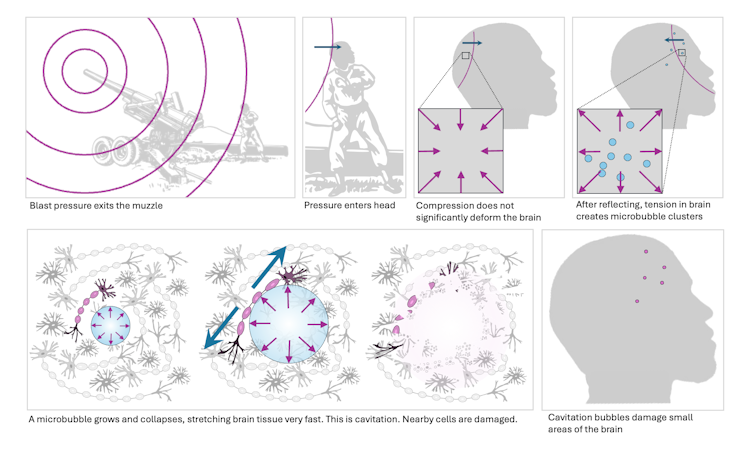 This diagram depicts how blast pressure from a gun can result in brain trauma. Alice Lux Fawzi and Manik Bansal, CC BY-NC-ND
This diagram depicts how blast pressure from a gun can result in brain trauma. Alice Lux Fawzi and Manik Bansal, CC BY-NC-ND
Cell death is the physical root cause of brain injury. In the lab, when the cells that make up brain tissue are deformed at a magnitude and rate beyond what they can withstand, they die – either immediately, as in the case of blast-induced cavitation, or slowly over six to 24 hours, as in most brain injuries from blunt impacts such as concussions.
In low-level blast exposure, the cavitation bubbles are very small, and the trauma is contained to the small area around them. However, repeated exposure to blasts can lead to an accumulation of these microtraumas, eventually reaching a volume large enough to cause significant and irreversible neurological symptoms.
Although evidence is mounting, it has yet to be fully proven that cavitation directly causes blast-induced traumatic brain injury. The hypothesis fits with post-mortem analyses of the brains of service members with a history of blast exposure. It also fits with the physics that link blast exposure to injury from tissue deformation.
Understanding the connection between blasts and cellular damage in the brain will help researchers develop better ways to protect against repetitive blast-induced traumatic brain injury.![]()
Alice Lux Fawzi, PANTHER Engineering Project Manager and Associate Director of the Center for Traumatic Brain Injury, University of Wisconsin-Madison and Christian Franck, Bjorn Borgen Professor of Mechanical Engineering and Director of the Center for Traumatic Brain Injury, University of Wisconsin-Madison, University of Wisconsin-Madison
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Contact us by email at thepanamanews@gmail.com
To fend off hackers, organized trolls and other online vandalism, our website comments feature is switched off. Instead, come to our Facebook page to join in the discussion.
These links are interactive — click on the boxes
>











